The MRI-guided biopsy
The MRI-guided biopsy provides a new type of procedure that is able to diagnose prostate cancer with a high level of accuracy.
In the case of an elevated PSA level or an abnormal digital rectal examination of the prostate a histological analysis of the prostate tissue is often recommended - this means the removal of a tissue sample for further investigation (biopsy). This is mainly carried out in the form of a transrectal ultrasound-guided biopsy based on a random principle. Using this method, false negative results can frequently occur, i.e. the cancerous areas in the prostate remain undetected, as the inserted biopsy needle does not hit the tumour. As a result, repeat biopsies need to be carried out as the abnormal findings from the digital rectal examination and/or the elevated PSA level continue to persist. Also, the situation can often be aggravated due to an inflammatory reaction in the prostate: this can be caused through manipulation by the biopsy needle or through the introduction of bacteria from the rectum during the course of the transrectal biopsy.
In the Clinic for Prostate Therapy, we follow a modified procedure for the efficient diagnosis of a potential carcinoma of the prostate. If there is clinical or laboratory suspicion of a prostatic carcinoma, a high resolution standardised MRI investigation (MRI: magnetic resonance imaging) of the prostate is carried out in accordance with the current guidelines for prostate diagnosis of the European Society of Radiology. Here, suspicious areas are identified and precisely located. In addition, information is gained on the spread of the tumour in the organ (capsule penetration), as well as on the infiltration of surrounding structures.
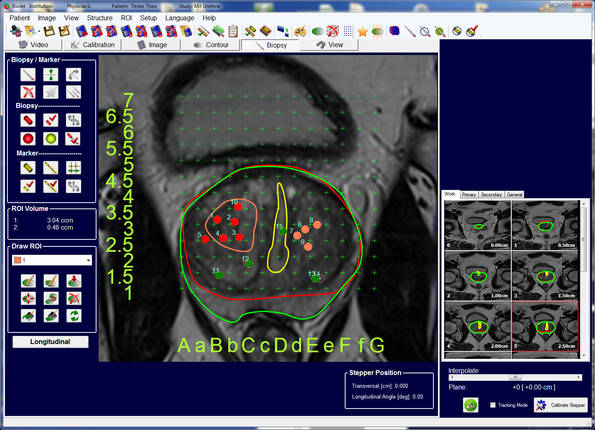
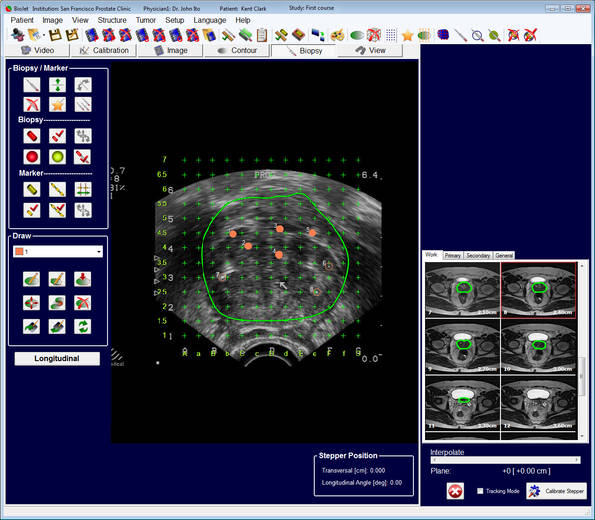
Furthermore, statements can be made with regard to the lymph node status. The information obtained in this way is used for a new, state-of-the-art method of combined imaging. Here, the MRI scans captured are superimposed on the current ultrasound images (so-called fusion imaging). As this type of investigation is carried out under a general anaesthetic, the patient is completely relaxed, feels no pain and there is no blurring of the image. The biopsy is therefore more precise than with practically any other procedure and it is no longer based on a random principle. Suspicious areas can therefore be reliably identified. The biopsy is carried out via the perineum, the area of skin between the scrotum and anus. The surgeon places a type of mathematical coordinate grid externally over the prostate and uses this to precisely access the areas that have been identified in the nuclear spin procedure as being abnormal. During the procedure, the puncture device is firmly fixed to the operating table and this increases the accuracy of the biopsy even further.
